Within the increasing older Australian population, there is a significant group at very high risk of developing complex oral diseases and dental problems—institutionalised older adults in Australian residential care facilities. Given that many older Australians are now retaining their natural teeth, rather than transitioning into removable dentures; dental health for older people is more complex today than ever before.1
Up until now, generally you would find that the majority of older people living in residential care facilities would have false teeth. It was very acceptable, until only about 15 years ago, for people to reach the age of 50-60 years and begin the normal ‘transition’ into dentures to replace their remaining teeth. This was typical because traditionally in dentistry, more teeth were removed as a way of treatment due to the absence of the materials and techniques of today. Therefore many Australian mouths would get to the point where there simply weren’t enough sound teeth left to support the jaw and function; and so dentures were a natural progression of life. Also traditionally, less attention was given to the gums holding the teeth in place so many people would lose their teeth to gum disease (going ‘long in the tooth’). We now know this can be easily prevented with regular scale and polishing visits.
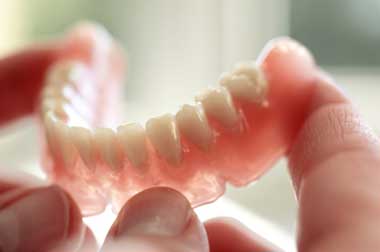
Nevertheless, dentures are quite easy for older people and/or carers to maintain because they are removable. All that is required is to take them out, brush them externally and soak them over night. Unfortunately, this is a practice that is too often not adequately done and although it may seem that because they are not natural teeth they don’t have to be looked after; if dentures are not removed and cleaned, a person can develop some very nasty secondary infections underneath the denture. Fungal infections are highly uncomfortable and can make an elderly person very sick. In turn this will affect eating habits, nutrient intake, immune function, general comfort, mood; and so is very significant to their overall wellbeing.
Research has demonstrated that cardiovascular disease, aspiration pneumonia, nutritional deficiencies and stroke are some of the possible complications that can result from poor oral health. Pain and social isolation are also frequently linked to poor dental health. Ageing can mean that people are less able to manage many customary daily living tasks that such as cleaning teeth that were once second nature. Studies have shown that many residents being admitted to residential care facilities have compromised oral health and high levels of oral disease that in many cases it is going unchecked. This will deteriorate if oral hygiene and mouth care planning is not undertaken and implemented.2
Now, Australians are keeping their teeth—and not just their teeth—heavily restored teeth with crowns, bridges, implants and partial dentures. This reflects a great improvement in the oral health of Australians however this is a much more complex situation to maintain in the residential aged care setting with medically compromised patients.
In the Australian residential aged care community, it is the carers who play an essential role in the delivery of oral hygiene care and the maintenance of residents’ oral health. Better integration of carers into oral hygiene care delivery and the timely identification of oral health problems are essential in improving residents’ access to and equity in oral health.1
In an effort to improve the level of oral health amongst people in residential aged care facilities (RACFs), The Better Oral Health in Residential Care Training project commenced in December 2009 and was rolled out to residential aged care homes nationally. The training aimed to provide an increased awareness of oral hygiene issues for the staff in daily contact with residents.
Two nurses or dedicated trainers in each aged care home, multi-purpose service and Indigenous flexible care service were offered training so that they in turn could train aged care workers in daily oral hygiene. There were 396 workshops delivered nationally, with 4,885 people trained from 2,809 aged care homes, multi-purpose services and Indigenous flexible care services. Training is now complete, but resources are available to support ongoing training in aged care homes.3
This is not enough. There are no funded systems in place to ensure that oral health care and professional management is accessible to institutionalised elderly people. It is the responsibility of the individual RACF and the individual carers. Due to lack of funding dental professionals continue to struggle to provide dental treatment, institute preventive oral care recommendations, and reduce the progression of caries and other oral diseases and conditions for their institutionalised patients, especially those with dementia.
We need to do more for this group in our community and this needs to change fast. At Bite Dental Studios we make a conscious effort to educate our patients, many whom are caring for older family members on the importance of their oral health and hygiene. It is important to be informed on this matter while there is much development and change yet to be done.